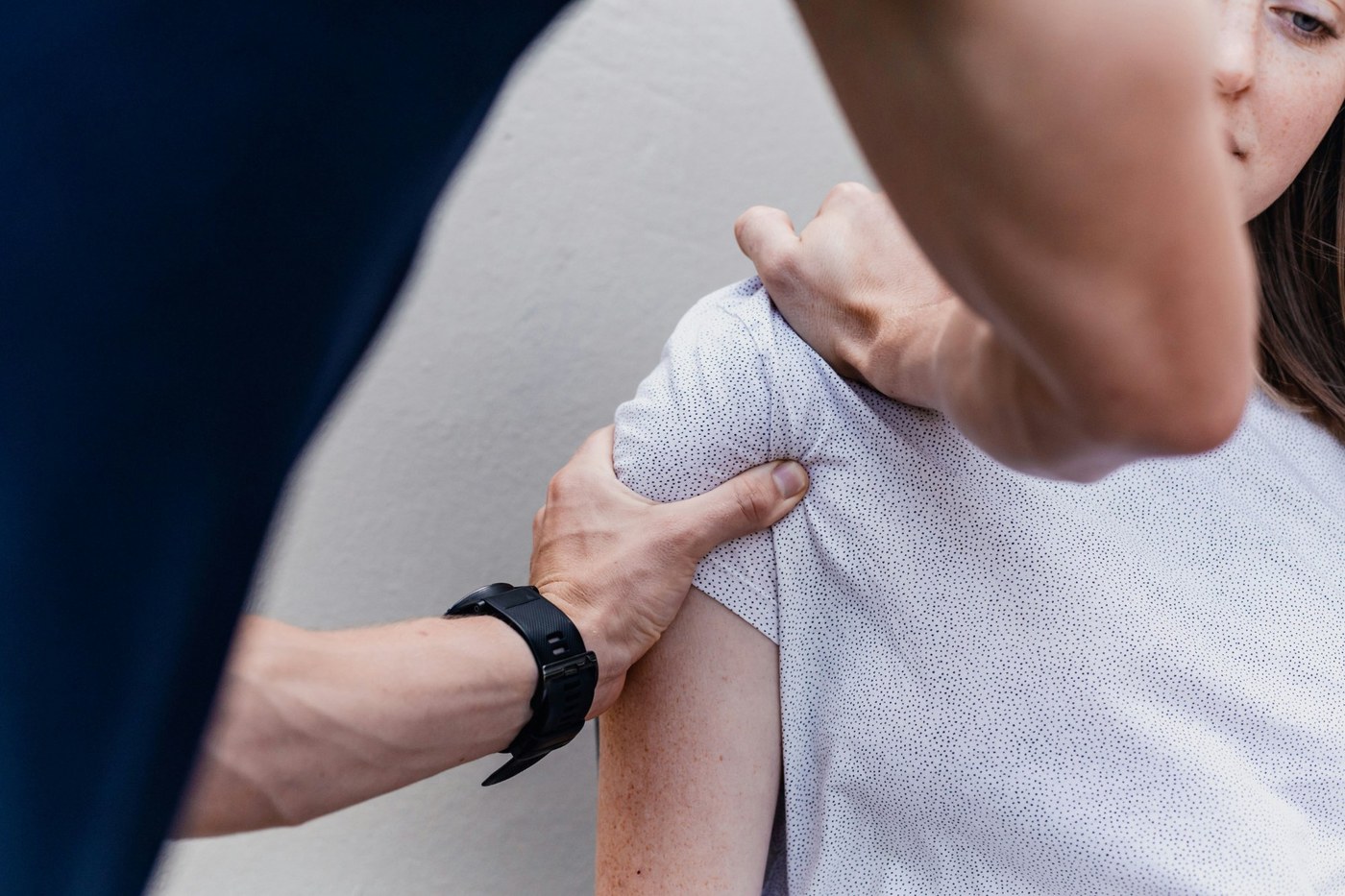
Frozen shoulder, or adhesive capsulitis, is a condition in which the capsule surrounding the shoulder joint becomes inflamed and thickened, gradually restricting movement. It typically progresses through three stages: a painful freezing phase, a frozen phase where movement is most restricted but pain may ease slightly, and a thawing phase in which movement gradually returns.
The full cycle can take anywhere from one to three years without treatment. With appropriate management, including osteopathic treatment, it is possible to reduce pain, maintain whatever movement remains, and accelerate recovery, particularly during the thawing phase.
Diagnosis matters here. Not all shoulder stiffness is frozen shoulder, and treating the wrong condition will delay recovery. Our assessment distinguishes true adhesive capsulitis from rotator cuff pathology, AC joint problems, and other presentations that can look similar.
Common symptoms
Gradual onset of shoulder pain, often worse at night
Progressive loss of movement in all directions
Difficulty reaching overhead, behind the back, or across the body
Pain that disrupts sleep, particularly lying on the affected side
A firm, hard end-feel when the shoulder is moved passively
Pain often felt in the outer upper arm rather than the joint itself